Diagnostics
At the Dry Eyes Clinic, we use a combination of diagnostic methods.
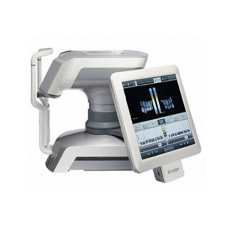
LipiView
The LipiView diagnostic device measures the lipid layers on your eyes, assesses your blink rate and takes pictures of your meibomian glands.
Lipid layers of 100nm are normal. Anything less can suggest meibomian gland disease.
Inadequate or poor-quality oil in the tear film makes tears evaporate too fast. Tear break-up time of less than 10 seconds is another indicator of meibomian gland disease.
Images of the glands show any blockages and/or gland atrophy/dropout. This helps the specialist identify whether glands need clearing and determine the severity of your disease.
Blinking is crucial for an optimal tear film. Poor blink rates affect the quality of the tear film and exacerbate dry eye symptoms.


Schirmer’s Testing
Schirmer’s testing is undertaken when we suspect that your dry eye is due to an aqueous layer deficiency.
Special filter paper strips are placed under your lower eyelids and you are asked to keep your eyes closed. After five minutes, the strips are removed and the degree of moisture in them is measured. Normal levels are anything over 15mm. Anything less than 10mm indicates reduced tear production. Less than 5mm is associated with severe dry eyes related to tear deficiency.
Symptom History
An important component of dry eye diagnosis is taking a full symptom history. Symptom patterns can help identify the underlying cause.
Examination
Examination will pick up the presence of underlying conditions such as rosacea, or the presence of a demodex mite infestation, which might need different or additional treatment.
Blood Testing
Depending on the results of a Schirmer’s test, blood testing may also be used to confirm or exclude Sjogren’s disease.

Further Investigations
If symptoms cannot be explained, our consultant ophthalmologist can offer further testing and imaging to determine other possible causes of your symptoms.
Demodex
Symptoms, Diagnosis and Treatment
MGD Treatments
MGD is a chronic condition and is not readily cured. However, with treatment, the symptoms can be relieved somewhat and progression slowed. Without treatment, blocked meibomian glands will eventually atrophy and drop out. As this is often non-reversible, early treatment for MGD is vital to prevent lasting damage to the meibomian glands.
There are multiple treatment options available, some of which are cannot be accessed on the NHS but are offered by the Dry Eyes Clinic. When you visit, our consultant will undertake cutting-edge diagnostic testing, take a full medical history and guide you to the most appropriate and effective treatment for your case.
What Is Demodex Folliculorum?
Demodex infestation is one of the causes of blepharitis and meibomian gland disease.
Small numbers of demodex mites usually live in the base on the eyelash follicle, coming out at night to feed off dead skin cells and usually causing no harm. However, if numbers increase too much or they live in the meibomian glands, they can create problems.

Eggs in the follicles can stretch them, leading to misdirected eyelashes. Deposits on the eyelashes leave them sticky or crusty and irritate the eyelids. These deposits also release toxins which trigger an inflammatory response
When they live in the meibomian glands, they cause meibomian gland disease. Oil glands in the lids can become blocked, causing dry and sore eyes.
Older people and those with rosacea tend to have greater numbers of demodex mites, making them more prone to blepharitis.

Demodex Treatment
Demodex is typically treated by cleaning the eyelids and eyelashes with tea tree oil. If this is not effective, then oral antibiotic treatment can be given. However, IPL treatment has also been found to be effective.
Treatment is required for a relatively lengthy period, as it usually eradicates demodex, but not their eggs, so it has to be continued until the eggs hatch and the new mites can be targeted.
Blepharitis & Meibomian Gland Dysfunction (MGD)
Causes, Symptoms and Treatment
Understanding Blepharitis and MGD
The term blepharitis refers to inflammation of the eyelid. The lids become red and irritated with dandruff- like scales forming on the eyelashes.
Some people may experience a single episode of blepharitis, which is easily treated. Other people, however, can suffer from chronic blepharitis. Blepharitis treatment will depend on the underlying cause.
Blepharitis is divided into two categories, based on where on the lid the inflammation occurs.
• Front or anterior part of the lid
• Back or posterior part of the lid
Meibomian Gland Dysfunction (MGD)
The meibomian glands are tiny glands in our eyelids, producing oils that form the top layer of the tear film. These oils prevent the water in your tears from drying out, making them essential for eye comfort as well as for visual acuity.
When the meibomian glands become blocked by hardened oil secretions, or there is narrowing/blockage of the ducts, they can no longer express oil. Eyelids become inflamed as a result of the blockage, and the lack of oil leaves the eyes dry.
A chalazion (meibomian cyst) may develop on the eyelid. This red bump may be painful initially but the pain will go away within a short time. Chalazions will usually go away by themselves once the blocked gland is treated.